Equine Diagnostic Services
With our on-site laboratory and advanced equipment such as the latest in digital imaging, endoscopy, gastroscopy, and other procedures, we are able to performa a number of diagnostic serices on our equine patients.

Laboratory Services
Our in-house laboratory is equipped with the Idexx Catalyst Dx and Idexx ProCyte. These instruments perform chemistry panels and complete blood counts, respectively. Results can be available within 20 minutes after the blood is drawn, depending on the type of blood sample obtained. The chemistry panel assesses liver and kidney function, and electrolyte concentrations can be included if needed. The ProCyte also performs cell counts on abdominal, thoracic, and synovial fluid.
Fibrinogen and serum amyloid A concentrations are two additional laboratory tests that are used to monitor the severity of an infection and its response to therapy. Each of these tests are performed on whole blood, with results available after 10 minutes.
In addition to the Catalyst Dx and the ProCyte, the laboratory also includes the Heska iSTAT, a point-of-care analyzer that performs blood-gas assessments. This instrument is critical to providing proper monitoring of anesthetized patients, as the blood oxygen and carbon dioxide concentrations can easily be obtained as needed throughout the anesthetic period. Neonatal foals with respiratory compromise are also monitored using the iSTAT.
Neonatal foals require special bloodwork to assess their Immunoglobulin G concentrations (IgG). A normal IgG concentration greater than 800 means the foal received enough good quality colostrum. This SNAP test takes just under 10 minutes to perform, and determines if the foal requires a plasma transfusion and/or antibiotics.
The final test performed in-house is a fecal floatation. This test shows the type of parasites (worms) in the manure, and how many. Results allow selection of the best deworming medication and the best frequency of deworming.
Digital Radiography

Digital radiography allows the veterinarian to review radiographs with such detail that even the most subtle of lesions are visible. Images may also be transmitted electronically anywhere in the world, shared with your veterinarian or specialist, or even taken home for review on a compact disc with no additional software requirements.
Digital radiography captures the image on a digital or phosphorus plate. Digital plates transfer the image to a computer and phosphorus plates are passed through a reader and then transferred to a computer, depending on the type of system used. Once in the computer, the images are saved as originally taken and can be adjusted for contrast and size. Images can be cropped, focused, edited, labeled and adjusted for detailed evaluation of soft tissue and bone.
Digital Ultrasound

The Toshiba Nemio provides unprecedented digital images of soft tissues located immediately beneath the skin or deep within the body. Frequencies as low as 2.5 mHz allow us to image the equine abdomen and chest, and higher frequencies of up to 14 mHz allow imaging of flexor tendons and suspensory ligaments.
The Nemio also provides us with color doppler technology. Color doppler provides real-time imaging of blood flow, allowing visualization of the heart and other blood vessels.
Ultrasound-guided surgery can be performed with confidence due to the excellent quality of the images provided by digital ultrasound.
Magnetic Resonance Imaging (MRI)

Why Would I Need An MRI?
- MRI evaluation is the only way to image soft tissue within the hoof capsule.
- The new MRI system decreases the scan time by 1/2 compared to the previous unit.
- An accurate prognosis can be provided using the information obtained from the MRI evaluation.

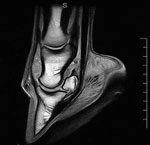
Magnetic Resonance Imaging (MRI) produces a radiofrequency pulse that affects the hydrogen atoms in the body. The computer detects how the hydrogen atoms are affected by the radiofrequency pulse, and generates a highly detailed image of bone and soft tissue.
MRI is best utilized when the problem can be narrowed down to a very specific region, for example the left front foot or right carpus. This is best accomplished by a detailed physical and lameness examination. The lameness examination may include temporary nerve blocks that help to localize the source of pain to a specific region. Once the pain is localized to a specific region, radiographs and ultrasound examinations are performed as needed. Pain can be caused by very small abnormalities in bones, tendons, or ligaments, and these abnormalities many of which are too small to be seen on radiographs or ultrasound. When radiographs or ultrasound are inconclusive but the area of pain is well defined, an MRI will often provide the necessary information.
Our MRI unit requires that the horse be anesthetized for approximately 60-90 minutes. General anesthesia minimizes any movement that would blur the image and decrease the information obtained by the MRI scan. During anesthesia, each horse’s heart is monitored with an electrocardiogram (ECG). Breathing is assisted and arterial blood pressure is monitored for the duration of the MRI scan.
Intravenous fluids are administered and the horse is supported on a thick foam cushion to prevent any damage to muscle tissue. Following completion of the scan, the images are sent electronically to a board-certified veterinary radiologist specially trained in equine MRI interpretation. Results are typically available within 6-24 hours. Appropriate therapy for your horse’s specific problem can then be recommended and implemented.
Nuclear Scintigraphy

As in human medicine, a bone scan involves the intravenous injection of a radioactive isotope. This isotope passes from the blood stream into soft tissues (muscles and tendons) and then into bone. Areas of inflammation or bone remodeling result in intense concentration of the isotope, i.e. “hot spots.”
Nuclear scintigraphy (bone scan) is a valuable tool in lameness diagnosis. The underlying cause of some lamenesses can be determined through a lameness examination, diagnostic nerve blocks, radiographs, and ultrasound. However, horses with more than one lame limb or with multiple problems in the same limb can be difficult to thoroughly diagnose by conventional methods. Additionally, lameness issues in the upper limbs (shoulder or hip), neck, back, and pelvis are often impossible to diagnose without nuclear scintigraphy.
Valuable information regarding inflammatory changes in and around joints, suspensory ligament desmitis, flexor tendon inflammation, and navicular syndrome can be obtained during the soft tissue phase of the scan. Scintigraphy can detect changes within tendonous structures prior to development of permanent damage. The bone phase of the scan is invaluable in the diagnosis of degenerative joint disease (arthritis), bone remodeling, stress fractures, and traumatic fractures.
Horses are hospitalized the day prior to the scan, and for a minimum of 24 hours after the scan to allow for dissipation of radioactivity. Following the scan, the areas of intense isotope concentration are evaluated via radiography or ultrasound and treatment recommendations are provided.
Videoendoscopy
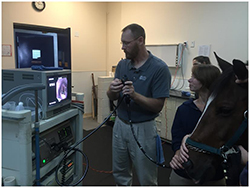
Endoscopic examinations of the upper-airway and urinary tract are performed using fiberoptic endoscopes of 1 and 1.9 meters in length. The images are seen in realtime on the video monitor. Videoendoscopy is an important tool in diagnosing respiratory abnormalities, sinus problems, and bladder abnormalities.
Dynamic Endoscopy

A dynamic endoscopy enables us to evaluate and analyze upper airway restriction problems during exercise. The system goes over the bridle and does not impact or impede the ability to control or use the horse as you normally would. This can be performed while riding or driving your horse.
The endoscope cable is placed into the horse’s nasal cavity with the camera tip positioned above the larynx. This placement gives an excellent view of the epiglottis and larynx at rest and during exercise. 2 hours of stable, high quality video can be recorded. The video can be viewed after the procedure while onsite or easily transferred to a computer.
Advantages of the procedure include the ability to perform the examination in the environment and with the same conditions in which the horse trains and competes. The procedure can be completed at a local racetrack and the Equine Specialty Hospital can assist with scheduling and coordination.
Gastroscopy

Gastroscopy is the evaluation of a horse's stomach and is an important component in diagnosing causes of colic, weight loss, inappetance, and poor performance. Gastric ulcers are most commonly located along the margo plicatus and the cardia. The margo plicatus is the separation between the top and bottom portions of the stomach, and the cardia is the area of the stomach where food enters.
A 3-meter endoscope is required to perform gastroscopy in horses. Prior to gastroscopy, the horse must be fasted for a minimum of 18 hours (no hay, grass, or grain) and should not receive any water for 4 hours prior to the examination. The horse is temporarily sedated for the examination, and the results are seen live via the camera.
Uterine Videoendoscopy
Uterine Videoendoscopy is performed in mares having difficulty conceiving a foal due to the presence of cysts, scar tissue, or tumors. Once the problem has been visualized on the videoendoscope, endoscopic-assisted laser surgery can be performed.
Myelography
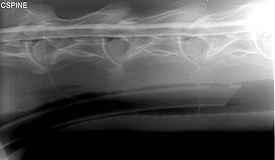
Myelography is a diagnostic test to determine if there is compression of the spinal cord in the neck of a horse. A myelogram is performed under general anesthesia. Cerebrospinal fluid is removed and replaced with a contrast agent, which outlines the spinal cord. A series of radiographs is taken with the head and neck in a neutral position, flexed and extended. The contrast agent outlines the spinal cord and makes it easier to detect subtle compressive lesions.
A myelogram is often the most important test in the diagnosis and consideration for surgery for horses with suspected cervical spinal cord compression (wobbler’s disease).
Advanced Lameness Diagnosis

Lameness is common in all breeds and uses of the horse. The Equine Specialty Hospital performs comprehensive lameness examinations in order to identify the source(s) of discomfort and provides you with detailed treatment options. Most lamenesses can be identified through traditional examination, conformation evaluation, flexion tests and local anesthesia (blocking). However, the hospital also sees a large number of horses that have complex lameness issues with either multiple sources of lameness in one leg, multiple limb lamenesses or severe neck, back or pelvic problems.
Digital radiography, digital ultrasonography, nuclear scintigraphy, and magnetic reasonance imaging (MRI) are all available at the Equine Specialty Hospital to help diagnose lameness problems. Once the problem has been diagnosed, a full complement of treatment options are available, including regenerative medicine and rehabilitation services.


